Sepsis remains one of the most formidable challenges in modern medicine. It is not merely an infection, but a catastrophic systemic failure where the body’s own immune response turns against itself, attacking healthy tissues and organs. Even with advanced treatments for the underlying infection, the mortality rates remain staggering: approximately 32% of sepsis patients die within 90 days, a figure that climbs to 39% for those entering septic shock.
However, a novel therapeutic approach—targeting a specific protein responsible for this hyper-inflammatory spiral—has shown significant promise in recent studies.
The Culprit: Galectin-3
For decades, researchers have studied a protein known as galectin-3. In a healthy body, this protein plays vital roles in regulating cell growth, division, and immune cell activation. Because of its versatile nature, it has been linked to various conditions, ranging from cancer to autoimmune diseases.
The breakthrough idea, championed by Isaac Eliaz of the Amitabha Medical Clinic and Healing Center, was to investigate whether galectin-3 acts as a primary driver of the lethal inflammation seen in sepsis. This hypothesis gained traction after studies revealed a consistent trend: higher levels of galectin-3 in the blood are closely correlated with higher mortality rates in sepsis patients.
A New Method of Treatment: Blood Filtration
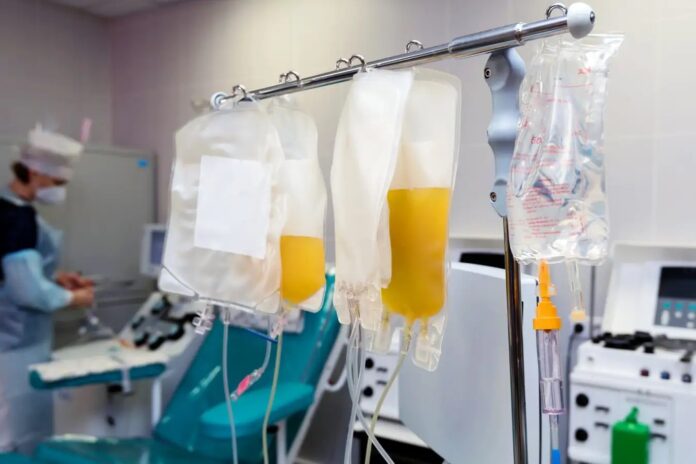
Rather than using traditional drugs to inhibit the protein, researchers have developed a mechanical way to physically remove it from the bloodstream. This process, known as apheresis, works through several precise steps:
- Extraction: A volume of blood is drawn from the patient.
- Separation: A centrifuge separates the blood into cells and liquid plasma.
- Selective Filtration: The plasma passes through a specialized filter containing antibodies specifically designed to capture galectin-3.
- Reintegration: The purified plasma and the patient’s cells are recombined and returned to the body.
Evidence from the Lab: Animal Success
To validate this technology, a research team led by Zhiyong Peng at Wuhan University’s Zhongnan Hospital conducted a series of rigorous tests. Their findings suggest that removing galectin-3 could significantly boost survival rates.
Key Research Findings:
- Human Correlation: In a study of 87 sepsis patients, researchers confirmed that those with the condition had significantly higher galectin-3 levels, which subsequently dropped in patients who survived.
- Rat Models: In experiments where rats were induced with sepsis, those treated with the filtration device had a 57% survival rate, compared to just 25% in the control group.
- Pig Models: In more complex miniature pig models, the results were even more striking. Despite receiving standard intensive care, the pigs treated with galectin-3 apheresis saw a 69% survival rate, while the control group saw only 27%.
The Path to Clinical Use
While these results are highly encouraging, the medical community remains cautiously optimistic. Experts, including Djillali Annane of Raymond Poincaré Hospital, note that while the innovation is significant, several hurdles remain.
Before this becomes a standard bedside treatment, scientists must:
– Fully understand the exact biological mechanisms of how galectin-3 drives sepsis.
– Replicate these results in independent studies.
– Test the efficacy in higher-order animals, such as primates, to better mimic human physiology.
“The results are consistent in the two animal models,” notes Annane, while emphasizing the long road ahead for standardization.
Looking Ahead
The transition from laboratory success to hospital reality is a massive undertaking. Eliaz Therapeutics is currently seeking the necessary funding to launch randomized clinical trials in humans, which are tentatively targeted for 2027.
Conclusion
If successful in human trials, galectin-3 apheresis could transform sepsis treatment from managing symptoms to actively neutralizing the biological driver of organ failure. This shift could potentially save millions of lives by halting the progression of septic shock before it becomes fatal.