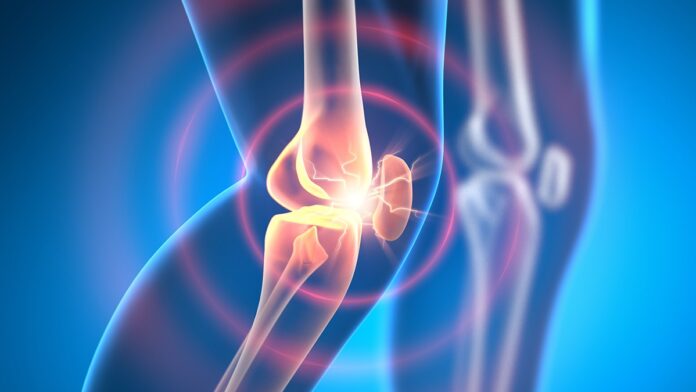
Osteoarthritis is a chronic, debilitating condition affecting hundreds of millions of people worldwide. Characterized by the progressive loss of joint cartilage, it leads to intense pain, bone decay, and significant loss of mobility. Currently, medical science offers no cure; patients are typically forced to choose between managing pain with medication or undergoing invasive, expensive joint replacement surgeries.
However, new research from the University of Colorado (UC) Boulder suggests a paradigm shift: moving from merely managing symptoms to actually reversing the damage.
A “Moonshot” Approach to Joint Repair
Led by chemical and biological engineer Stephanie Bryant, a research team has developed an experimental, slow-release drug-delivery system. Unlike traditional treatments that focus on inflammation, this method aims to reprogram the body’s own biology.
The mechanism works by injecting a specialized substance into the damaged joint that “coaxes” the body’s existing cartilage and bone cells to begin the repair process. In animal models, this has demonstrated the ability to reverse osteoarthritis symptoms within just a few weeks.
The research is moving through several distinct stages of development:
– Phase 1 (Completed): Initial animal experiments demonstrating the reversal of joint decay.
– Phase 2 (Upcoming): Intensive testing focused on safety and toxicology to prepare for human application.
– Long-term Goal: The development of different “implant” options tailored to the four distinct stages of osteoarthritis—ranging from mild cartilage thinning to the severe “bone-on-bone” contact that causes extreme swelling and stiffness.
The Broader Landscape of Osteoarthritis Research
The UC Boulder team is not working in a vacuum. The global scientific community is currently exploring several different avenues to tackle this widespread epidemic:
- Protein Targeting: Researchers at Stanford University have identified a specific protein linked to age-related cartilage loss, suggesting that neutralizing this protein could protect joints as we age.
- Metabolic Intervention: Interestingly, semaglutide (the active ingredient in drugs like Ozempic) has shown potential in boosting cell metabolism, which may help maintain healthy cartilage.
- Preventative Care: While biological breakthroughs are pending, clinical consensus remains that regular exercise—which strengthens supporting muscles and circulates nutrient-rich fluids through the joints—remains a vital defense against cartilage depletion.
What Lies Ahead?
The transition from animal success to human application is a rigorous process. The UC Boulder team hopes to begin human clinical trials within the next 18 months, contingent upon the results of their upcoming safety studies.
This research is being supported by the NITRO program, an initiative of the Advanced Research Projects Agency for Health (ARPA-H) under the US Department of Health and Human Services.
“Our goal is not just to treat pain and halt progression, but to end this disease.” — Stephanie Bryant, UC Boulder
Conclusion
While human trials are still on the horizon, the ability to trigger biological repair via a single injection represents a significant leap toward making osteoarthritis a treatable, rather than a permanent, condition.